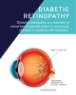
Understanding diabetic retinopathy
Diabetic retinopathy is a progressive condition that affects people with diabetes. The disease starts when the tiny blood vessels around the retina become blocked or damaged, causing them to leak fluid into the eye. As the blood vessels heal, the resulting scar tissue can affect vision. Retinopathy can worsen slowly over several years, leading to secondary conditions like macular oedema, which can also damage vision.
Diabetic retinopathy is one of the leading causes of blindness in New Zealand. Diabetic people are at risk of developing the condition, but it’s more likely in those who have had the disease for years and who rely on insulin to manage it.
If you have diabetes, it’s crucial to have your eyes checked for early signs of retinopathy, as it can develop without symptoms.
Click here to view a video describing early symptoms of Diabetic Retinopathy such as blurriness or floaters, which can lead to severe vision loss if left untreated.
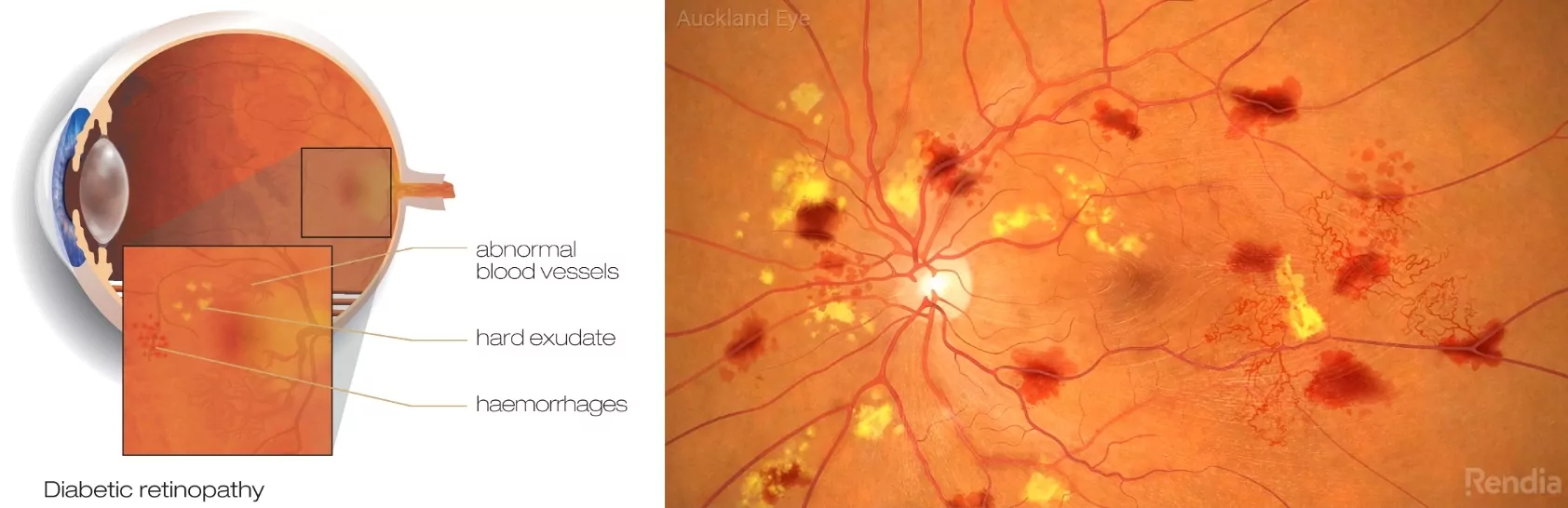
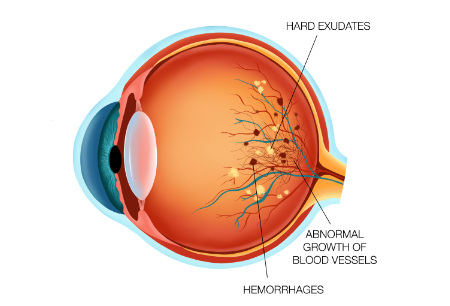
Causes: damage, scarring and swelling
The retina is the light-sensitive layer at the back of the eye that sends visual signals to the brain. The macula is the central portion of the retina. It delivers the sharpest vision in the central field. Diabetic retinopathy can affect these crucial parts of the eye, causing severe vision problems over time.
The condition is caused by swelling and leaks in the retina’s blood vessels. These leak fluid or blood into the retina, leading to large floaters in the eye and blurred vision. When the blood vessels heal, they leave scar tissue on the retina, also affecting vision. Severe scar tissue on and around the retina can also pull it out of place or cause it to detach.
Later in the process, the macula itself may swell and seriously affect vision and, in some cases, may cause blindness.
Non-proliferative retinopathy
In this early stage of the disease, tiny blood vessels and minor leaking may be present, but you are unlikely to experience any signs or symptoms. Even at this point, it is possible to develop macular oedema, or swelling of the macula, which can be particularly dangerous for vision.
Proliferative retinopathy
As the condition progresses, it becomes proliferative as the eye grows new blood vessels to replace the damaged ones. Unfortunately, because these new blood vessels tend to be damage-prone, leaking, scar tissue and blurred vision often worsen. You may need treatment to remove blood vessels or scar tissue at this stage.

Symptoms and diagnosis
While diabetic retinopathy can reach a critical stage without apparent symptoms, you may notice vision changes and other signs. Symptoms include:
- Blurred vision, which may occur when blood sugar levels fluctuate
- Floaters – transparent spots that drift across your field of vision
- Flashes – tiny flashes of light at the edges of your visual field
- Sudden loss or worsening of vision
Even if you don’t notice symptoms, it’s important to have regular check-ups if you have diabetes. After taking a full medical history, your ophthalmologist will run several tests. These may include:
- Full eye examination
- Vision tests
- Retinal examination using a bright light
- Photos of the retina
- An optical coherence tomography (OCT) scan that looks for swelling in the macula
- Checking fluid pressure in the eye
- Fluorescein angiography – used rarely, this involves injecting dye into the arm and examining the eye using UV light.
Minimising the risk of diabetic retinopathy
People with diabetes risk developing retinopathy, but there are ways to lower your risk. The most effective method is carefully managing your diabetes, avoiding uncontrolled blood sugar levels and maintaining a low HbA1c. Of course, this is easier said than done.
Diabetic retinopathy often worsens during pregnancy, so you should talk to your eye specialist about extra monitoring and management if you are pregnant.
Other strategies include:
- Regular eye checks, including retinal exams, so you can treat symptoms as early as possible
- Close self-monitoring of diabetes, with help from your GP or specialist
- Avoiding smoking, which raises the risk of eye disease

Treatment options
While there is no cure for diabetic retinopathy, it is possible to treat the symptoms of the disease and prevent loss of vision for most people. The best treatment will depend on the progression of your disease, how the symptoms affect you and other conditions or medical issues.
Anti-VEGF injections
Anti-VEGF (vascular endothelial growth factor) medication works by suppressing the growth of abnormal blood vessels characteristic of retinopathy. It reduces macular swelling in around 50% of patients and improves vision at similar rates.
The medication is injected into the sclera (or white of the eye) with a local anaesthetic or numbing cream to minimise discomfort. Treatment is ongoing, starting with injections once a month and reducing the frequency depending on the response. Some patients with severe retinopathy may need injections for years.
After the treatment, you may have eye irritation at the injection site, but this usually resolves quickly.
Corticosteroid Injections
If you have severe macular oedema or other serious symptoms, you may require steroid injections. Corticosteroids, which have strong anti-inflammatory properties, are injected into the eye to reduce swelling. The process is similar to anti-VEGF treatment and may need to be repeated regularly.
Vitrectomy
This surgical treatment is used for severe scarring or bleeding inside the eye. During the surgery, the surgeon makes tiny slits in the sclera, or white of the eye, and uses suction to remove the jelly-like vitreous body and any blood or fluid. Once the vitreous body is gone, the surgeon uses a laser to remove scarring or damaged blood vessels on the retina. Finally, the eye is filled with saline fluid or gas, which it gradually absorbs as it replenishes the vitreous body.
Recovery and results
A vitrectomy is usually safe but does require two to four weeks of recovery. The eye may be scratchy and sore for a while. Occasionally, bleeding may recur, and a second surgery may be needed. For most people, a vitrectomy effectively prevents severe vision loss.
Laser photocoagulation
Although used less frequently than other treatments, laser photocoagulation can sometimes be an effective way to treat the multiple blood vessels that appear during proliferative retinopathy. During laser treatment, numbing drops are applied and blood vessels are targeted with a laser, causing them to shrink and seal off. Fewer blood vessels mean less bleeding and scarring in the eye, preventing further damage to vision.
Click here to view this video which gives an overview of various diabetic retinopathy treatments and healthy living options.
Get regular eye checks
While diabetic retinopathy is a complicated and dangerous disease, safe, effective treatment options are available. Most importantly, getting regular eye checks is crucial if you have diabetes, so your specialist can recommend the right treatments and help you avoid the worst effects of retinopathy.