Understanding the epiretinal membrane
An epiretinal membrane (ERM) is semi-translucent scar tissue that forms on the retina’s inner surface. When it develops over the macula (the central area of the retina), it can change its natural shape, leading to blurred and distorted vision. In most cases, people with ERM don’t have any symptoms in the affected eye and only discover it during a routine retinal exam.
Vision problems and clarity issues
Most ERMs are ‘idiopathic’, meaning the condition appears in healthy people who have no other trauma or diseases of the eye or surrounding tissues. These cases are usually associated with age-related changes in the eye, such as shrinkage and contraction of the vitreous gel. Other contributing factors include eye inflammation, retinal tears or detachment, trauma to the eye and certain medical conditions like diabetes.
Signs and symptoms
- Blurred or distorted central vision
- Wavy or distorted lines – straight lines may appear wavy, bent or distorted
- Reduced visual acuity – the ability to see details may be diminished
- Double vision out of the affected eye
- Micropsia – objects appear smaller than their actual size
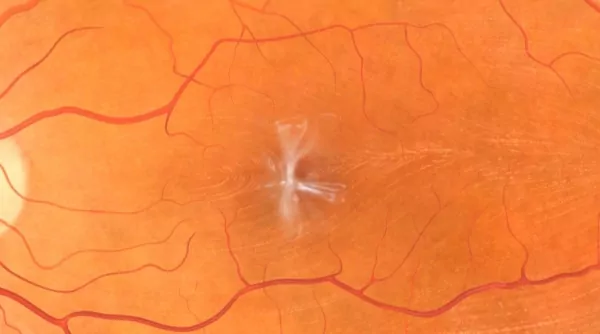
Epiretinal membrane can cause distortion of the macula
Diagnosing epiretinal membrane
Routine eye examinations are usually needed to detect ERMs. Your ophthalmologist will thoroughly examine your eye and retina to identify abnormalities. To assess the true severity of an ERM and find the underlying causes, optical coherence tomography (OCT) retinal imaging may be needed. OCT is a non-invasive imaging technique that gives detailed cross-sectional images of the retina. It allows your ophthalmologist to see the thickness and structure of the retina, including the presence of an ERM and its impact on the retinal layers.
Treatment options
Your ophthalmologist needs to know your complete medical history to plan the best treatment. Disclose all health problems, especially the following:
- Any allergies or bad reactions to antibiotics, sedatives, anaesthetic drugs or any other medicine, including aspirin
- Any blood disorders
- Heavy bleeding when you are injured or have surgery
ERM surgery
Once diagnosed, a surgeon will look at the likely cause and rule out any secondary causes. From there, they will evaluate whether the removal of the ERM will improve your visual function. Seek your surgeon’s advice about stopping any blood thinning therapy, which may increase the risk of bleeding during and after surgery.
Anaesthesia
ERM surgery usually involves a local anaesthetic to numb the eye, along with a mild sedative. This combination means you’ll feel relaxed but not drowsy, and without pain. Sometimes, general anaesthesia is used.
Cost of treatment
Our surgical bookers can advise you about approximate cost of the surgery including any out-of-pocket expenses. The exact amount may vary due depending on the nature of surgery. Alternatively, you can ask your surgeon to refer you to the public hospital.
Recovery after surgery
The surgery usually takes less than 60 minutes and you can go home the same day. You may feel mild discomfort several days following your surgery, including swelling, redness, and scratchiness. Paracetamol is usually sufficient to help with this.
You will usually be given anti-inflammatory and antibiotic eye drops to use for a few weeks after surgery. Avoid bending, strenuous activity and lifting heavy objects for at least one week, and be sure to attend your follow-up appointments.
If air or gas has been used during surgery, you must avoid air travel and high altitudes for up to two months because changes in air pressure can damage your eye. Before resuming air travel, consult your ophthalmologist.
Treatment outcomes
Visual recovery can be slow and typically depends on the length of time the ERM was present. Expect vision to be blurry at first but to improve as the retina heals gradually. Many patients report that vision steadily improves over three to six months, with some patients reporting ongoing improvements at 12 months.
Possible complications
While ERM surgery is very safe, there are occasional complications. Talk to your ophthalmologist if you’re concerned.
- Retinal tearing – may require laser treatment or lead to retinal detachment, which can cause vision loss
- Cataracts – the natural lens normally goes cloudy with age; however this process is accelerated following ERM surgery
- Endophthalmitis – Infection of the eye
- No change or worsening of vision – This is despite successful removal of the ERM
- Elevated pressure – intraocular gas can cause higher pressure inside the eye
- Scarring or glaucoma – can cause reduced vision or blindness.
- Hypotony – low intraocular pressure
- Excessive bleeding – into the vitreous cavity or other eye structures
- Damage to the optic nerve
- Retinal injury – due to a surgical instrument
For more information or to book your consultation, please get in touch on 0800 25 53 93











