Understanding cataracts
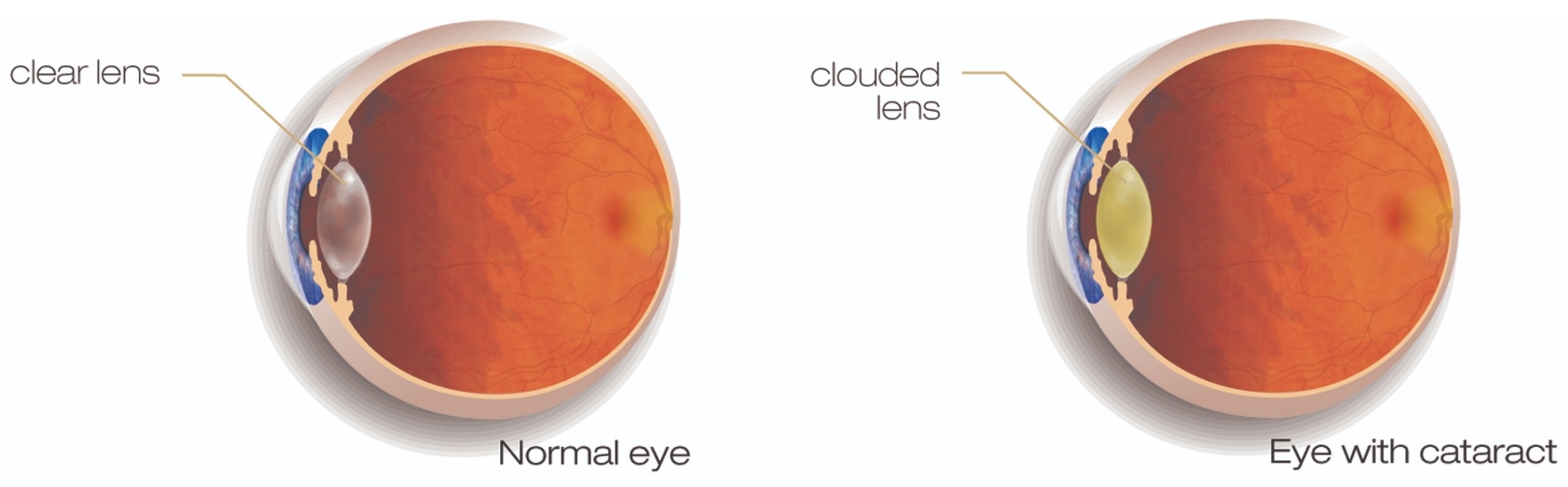
A common result of ageing, cataracts develop in roughly 50% of people by age 60. The condition results from protein building up in the eye, clouding the lens and restricting the light that reaches the retina.
Vision can be affected in several ways – including blurring, issues with focus, light sensitivity and problems seeing in low light. Cataracts range from minor and manageable to large enough to obscure vision and interfere with everyday activities.
Causes: ageing, eye trauma, genetics
Although cataracts are a natural result of ageing, happening to almost everyone aged 70+, some factors can cause them to develop earlier or have a greater impact on vision.
If you have a history of eye infections or diseases, trauma to the eye or significant UV damage, diabetes or other long-term health problems, or family members with cataracts, you may be more likely to develop them. Some medications, particularly steroids, can also increase the risk.
Although cataracts come with ageing, some factors can cause them to develop earlier or have a greater impact on vision.
Risk factors include:
- History of eye diseases or infections
- Previous trauma to the eye
- UV damage
- Diabetes or other chronic conditions
- Use of medications, particularly steroids
- Family history of cataracts

Symptoms to watch for
- Cloudy, blurry vision – as if you’re looking through a mist or net curtain.
- Increasing light sensitivity
- ‘Halo’ effect around bright lights.
- Poor or worsening night vision
- Monocular double-vision – seeing multiple images in one eye
- Frequent prescription changes
- Dulling or darkening of colours
Diagnosis and treatment
Diagnosis involves visual acuity and contrast sensitivity tests, pupil dilation and examination under magnification.
Treatment for cataracts
You only need surgical intervention if cataracts seriously affect your vision and interfere with daily life. For example, if you’re finding it difficult to work, read or drive, your specialist will likely recommend surgery.
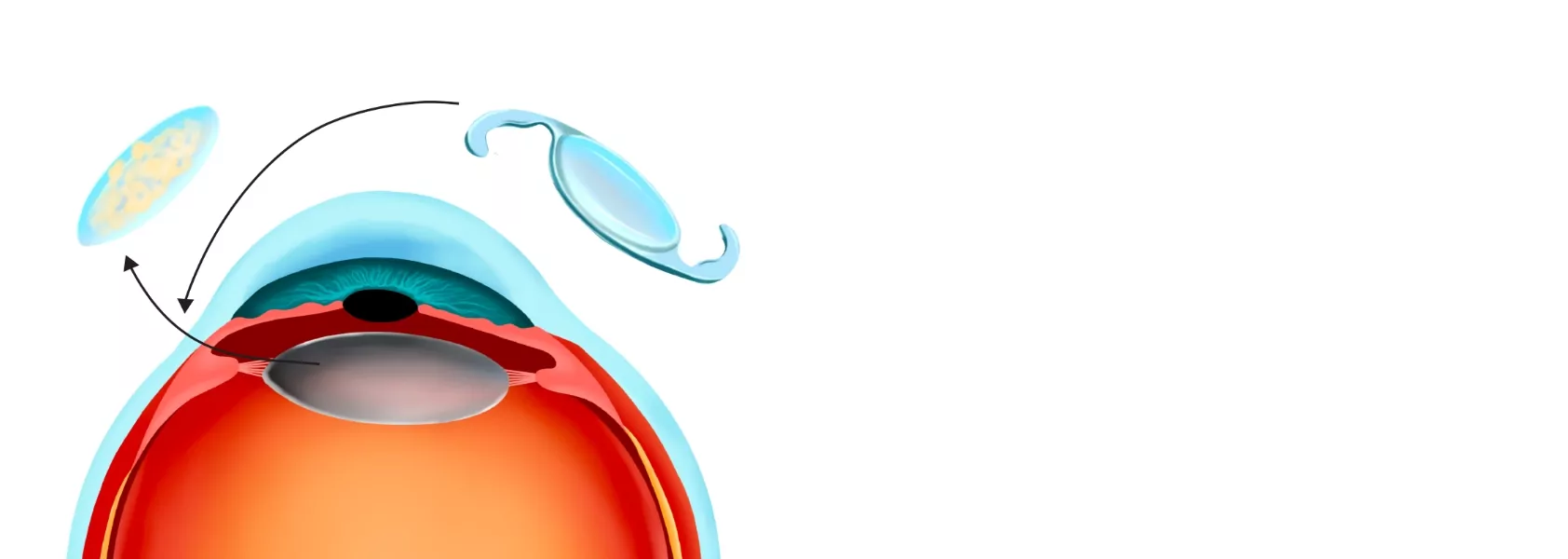
Cataract surgery involves removing the clouded lens and replacing it with an artificial version called an intraocular lens (IOL). The IOL fits into the space left by your natural lens – you won’t be able to feel it or tell it’s there. In most cases, IOL implants will last for the rest of your life. IOLs can even be customised to suit various vision needs, much like contacts or glasses, with bifocal, trifocal, monofocal, fixed focus or extended depth of focus available.

Surgery techniques
Small-incision surgery (phacoemulsification)
Using a high-powered microscope, your surgeon will make a 3mm incision near the edge of your cornea. A probe is inserted to break the clouded lens into smaller pieces using high-frequency vibrations, so it can be gently suctioned out.
Once the clouded lens has been removed, the surgeon will insert an IOL through the probe where it unfolds to fit.
Large- incision surgery
If small-incision surgery isn’t suitable for your situation, your surgeon may recommend a large-incision method. This involves making a larger incision to extract the clouded lens and replace it.
Recovery and risk
After your surgery, you will be monitored for a few hours before you can leave. Your eye will be covered with a shield, and you may be recovering from anaesthetic, so you will need someone to drive you home.
During recovery, bright light may seem particularly intense, so wear sunglasses for protection if needed. Avoid rubbing or touching your eye, and try not to do anything that will cause rapid movement or shock. Some patients may need to take paracetamol or other over-the-counter medications for pain.
Although cataract surgery is safe, there is a slight chance of complications. Your surgeon will be able to talk you through the risks.